|
12/24/2023 0 Comments Moca test pdf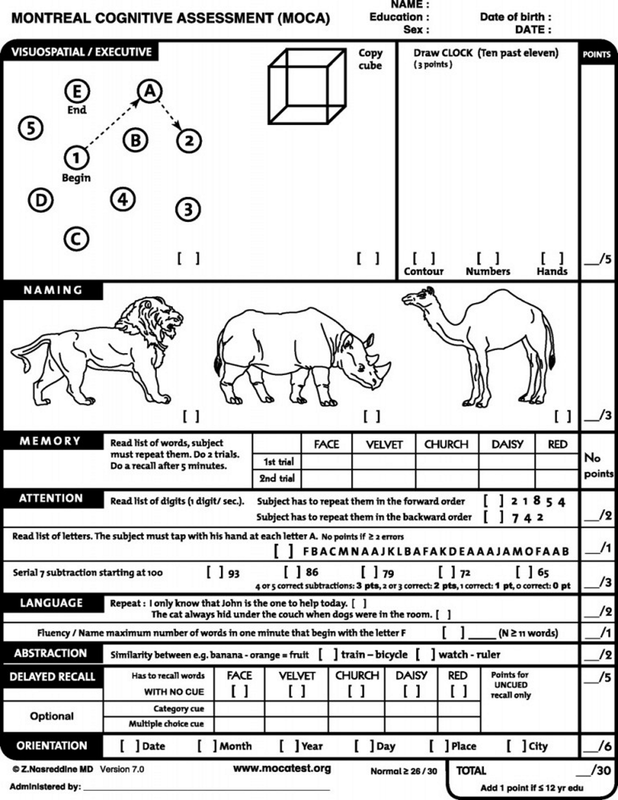 
Here, patients with a wide variety of etiologies of possible cognitive impairment (CI) are presented-including major depressive, schizophrenic- and bipolar-disorders. The MoCA can reduce referrals substantially (50%) by selecting who don’t need further work up in a memory clinic, even if they were suspected of CI after initial assessment.ĭiagnosing, as well as the guidance and treatment of dementia, including Behavioural and Psychological Symptoms of Dementia (BPSD), is often done in old age psychiatry which, at least in the Netherlands, make up to 25% of all memory clinics (Verhey et al., 2010). The AUC of MD against non-demented (MCI + NoCI) was 0.83(95%CI: 0.78–0.88) resulting in 90% sensitivity, 65% specificity, 50%PPV and 94%NPV at a “best” cutoff of <21 according the Youden index and respectively 0.77(95%CI: 0.69–0.85), 56%, 73%, 90%, 28% for CI (MD + MCI) against NoCI at <21.Ĭonclusion: 90% of individuals with a MoCA of <21 will have CI (MD + MCI), while 94% with a MoCA of ≥21 will not have dementia. Results: The mean MoCA scores differ significantly between the groups: 24(SE. The reference standard was the consensus-based diagnoses for MD and MCI, adhering to the international criteria and using suspected patients, but without CI as comparisons (NoCI). Method: The MoCA is validated for identifying MD and mild cognitive impairment (MCI) in a cohort of patients suspected of cognitive impairment (CI) after initial assessment in old age psychiatry. A validated instrument that can triage patients when they are suspected of mild dementia (MD) is necessary to optimise referrals. Objectives: Diagnostic pathways are limited.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
